
Historical perspective: from native to prosthetic joints This narrative review provides an overview of these factors and its possible influence on the threshold and accuracy of the WBC count and PMN% in synovial fluid for PJIs. Factors such as joint site, co-morbid conditions, the causative microorganism and the duration of infection, in addition to pre-analytical laboratory variables, may influence the optimal cut-off result 13. Its sensitivity, specificity and diagnostic accuracy depends on the threshold that is applied. The test can be performed relatively easily in the preoperative diagnostic work-up. One of them includes the synovial white blood cell (WBC > 3000cells/µL) count and its proportion of polymorphonuclear cells (PMN% > 70). 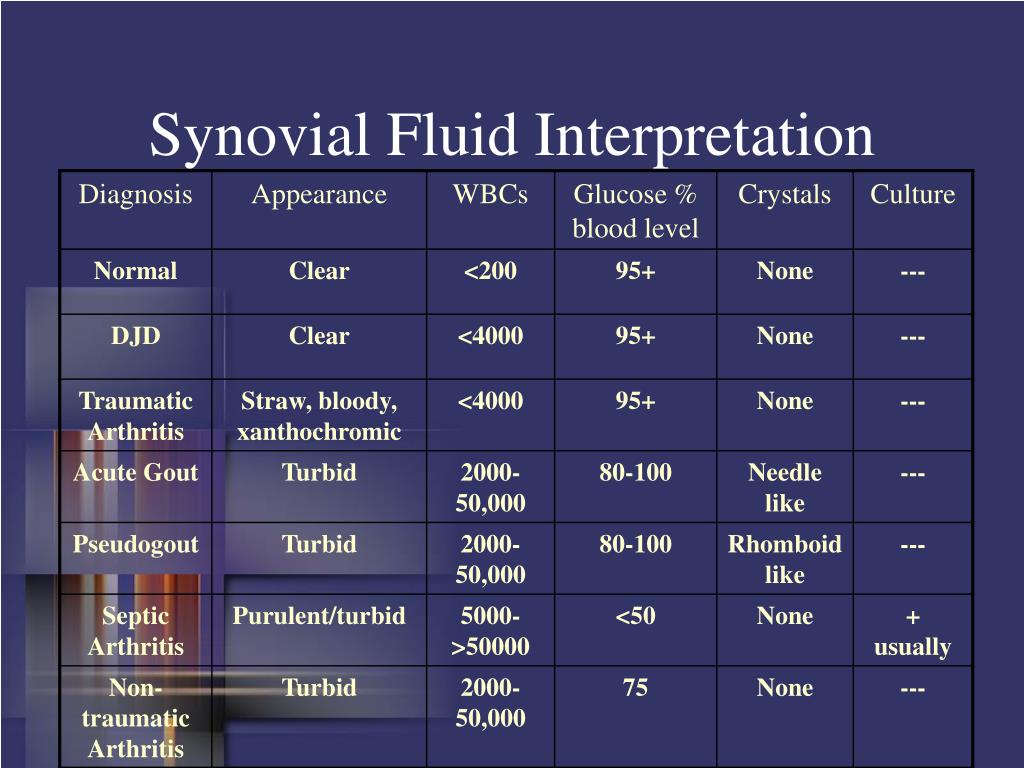
Criteria for the diagnosis of PJI have been proposed by the Musculoskeletal Infection Society (MSIS) and the International Consensus Meeting (ICM) 10 - 12. It is critical to distinguish between septic and aseptic failure preoperatively, as arthroplasty exchange of a missed PJI leads to subsequent failure 8, 9. Because there is no single and absolute test to confirm or exclude infection 1 - 7, patients' history, physical examination, joint specific x-ray or other types of imaging, histology, culture and inflammatory markers should all be taken into consideration for diagnosis. The diagnosis of a periprosthetic joint infection (PJI) is challenging especially for chronic PJIs.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
